
Some of the links on this page may link to our affiliates. Learn more about our ad policies.
Guide to Dialysis and Kidney Disease
Updated on: December 2022
Reviewed by: Nancy Leahy, RN, APNP

Kidneys are among the most vital organs in our bodies. They are the driving force behind filtering all the blood in your body. Kidneys draw the waste out the blood and help keep fluid and electrolyte levels regulated, pushing all the bad material out through urination. You have two kidneys, one on each side of your spine below the rib cage, and you may not notice anything wrong with them—even if just a small fraction of your kidneys are working.
There may come a point, though, after years of having kidney disease, where your kidneys stop working properly altogether. This could be from damage from having low quality blood flow through them or other reasons, and it’s when you are in immediate need of help. This is where dialysis comes in. It’s a treatment that helps filter your blood for you when your kidneys can’t. Here’s more information about kidney disease in seniors.
Find What You Need
Kidney Disease
To understand what a treatment like dialysis does, you first need understand why you would be getting it done in the first place. To reach the point of needing dialysis, your kidneys must stop functioning to the point where they can no longer filter the blood in your body on their own. This occurs during the final stage of chronic kidney disease (CKD), the main disease that causes your kidneys to deteriorate to the point where they can’t be used anymore.
To reach the point of needing dialysis, your kidneys must stop functioning to the point where they can no longer filter the blood in your body on their own.
CKD is a chronic condition that can develop very quickly or over the course of many years. But in either situation, the end result is the same: your blood needs to cleansed, and you need to seek help in order to do that.
There are five stages of chronic kidney disease in seniors, each varying on how much blood and waste your kidneys can filter per minute. Doctors may test your blood to see the levels of creatinine—a waste product—in your blood to see if kidneys are filtering the blood properly.
The most mild stage (stage 1) occurs when kidneys aren’t functioning quite normally, but they can still filter 90 mL of blood per minute. The stages trickle down with varying levels of filtration until stage 5—end-stage renal disease (ESRD)—where your kidneys absolutely need help filtering blood on their own.
Kidney Failure, by the Numbers
It’s predicted that about 14 percent of the population is at some level of chronic kidney disease, and 650,000 Americans are in the final stage—ESRD—of the disease. Many of those 650,000 are elderly. One study noted that “individuals 65 years old and older now comprise the most rapidly growing segment of the ESRD population in wealthier countries.” Not only is the population growing, but it’s also predicted that just under half of people over the age of 65 are at some stage of CKD, meaning they’re at risk of developing ESRD soon.
650,000 Americans are in the Final Stage of Kidney Disease
According to the University of California, San Francisco, the prevalence of ESRD is increasing at a rate of 5 percent per year, meaning that more than one million people will be in dire need of kidney treatment by the year 2027.
Not only are the numbers of people with ESRD increasing, the likelihood of someone developing the disease is highly skewed based on race. According to the American Kidney Fund:
- African Americans are four times more likely to develop ESRD than white people
- Native Americans and Asian Americans are about 1.5 times likely to develop ESRD than white people
- Hispanics are also about 1.5 times more likely to develop ESRD than non-Hispanics
The Kidney Fund also reports that, while women are more likely to be at some stage of chronic kidney disease, men are 50 percent more likely for their CKD to develop into ESRD than women.
Causes
The list for the causes of kidney failure is long, and many of the causes revolve around the quality of your blood, which then affects everything else in your body. Having any of the following can increase your likelihood of developing kidney disease:
High Blood Pressure
One of the leading causes of kidney failure, high blood pressure can damage nerve endings and blood vessels within the kidney that can stop it from working properly, according to the National Institute of Diabetes and Digestive and Kidney Diseases.
Diabetes
Another one of the leading causes of kidney failure, diabetes means your blood sugar levels are too high, which can then affect the quality at which kidneys can filter the necessary waste out of your blood. The NIDDK says that one in three of diabetes patients has chronic kidney disease.
Glomerulonephritis
A disease that “damages the kidneys’ filtering units” and may be acquired by being passed down through generations.
Family History of Kidney Disease
You’re more likely to develop kidney disease if someone else in your immediate family has dealt with the issue in the past.
Heart Failure
If something is wrong with your heart, that means there’s something wrong with the blood flowing through it, which can then affect every other organ in your body, including your kidneys.
Symptoms
The only true way to know if your kidneys are decreasing in their ability to function is going to the doctors and getting the right tests done. Before your kidneys reach the advanced stages of failing, there aren’t many symptoms that indicate that anything is wrong. But once chronic kidney disease starts to really take effect, some of the symptoms include the following:
- Nausea
- Headaches
- Change in urination patterns
- Chest pain
- Sleep problems
- Weight loss
- Numbness
- Dry skin
If your kidneys aren’t working properly, it directly affects the quality of your blood, which travels all around the body. Thus, the effects of cokidneyfailure can be felt everywhere. If your kidneys reach this point, this is where dialysis comes in.
Getting Tested for CKD
There are certain tests doctors conduct to figure out how well your kidneys are functioning. Figuring this out will help doctors pinpoint exactly what stage you’re at with chronic kidney disease and how to treat it. Some of these tests include:
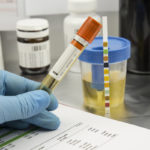
Urinalysis
Doctors test your urine to see what your kidneys are or aren’t filtering out.
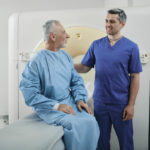
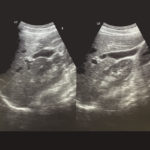
CT Scans/Ultrasounds
Taking pictures of your kidneys can help doctors see physical damage to your kidneys, which can indicate a decrease in their functions.
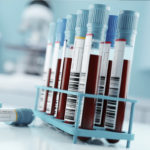
Blood Samples
This helps doctors see what type of waste is being filtered out of your kidneys or if not enough is being filtered out. Doctors will analyze amounts of nitrogen or creatinine in your blood and see if levels are too high or low.
Kidney Biopsy
Doctors can perform a small, non-sedative biopsy to gain access to kidney tissue, which can then help reveal the exact type of kidney disease you have and how severe it is.
The two solutions for kidney failure are dialysis or a transplant, but the transplant list is so long for kidneys that you need the former as an immediate solution. It’s been reported by the UCSF that there are about 100,000 people on the kidney transplant list, while less than 20,000 kidneys are available per year.
What is Dialysis?
Dialysis is the primary form of treatment for kidney disease, given the lack of healthy replacement kidneys available to the public through transplants. The NIDDK says that of the estimated 650,000 people who have reached ESRD, about two-thirds of them are on dialysis. The other third have been able to find a kidney via transplant.
429,000 People Out Of Those Who Have Reached ESRD Are On Dialysis
Dialysis is the process of filtering your blood when your kidneys can’t. It’s a treatment where an outside device acts as your kidneys. The sessions can be done while you’re still able to be mobile, or they may render you immobile and last for hours on end.
Types of Dialysis
There are two main types of dialysis, both with the main goal of cleaning your blood. But each treatment style differs per your personal preference, or your physical ability to take part in the process of cleaning your blood. Let’s take a look at the type main types of dialysis treatment.
Hemodialysis
Hemodialysis is the most common type of dialysis, with almost 90 percent of dialysis patients taking part in this treatment style. Hemodialysis is also the most immobile and inconvenient form of dialysis.
Treatment begins with a small surgery to get doctors consistent access to your blood vessels, with a small incision usually being placed in an arm or a leg. Then, you are connected to a machine called a “hemodialyzer,” which basically acts as an artificial kidney outside of your body. The blood is transferred from your body into the hemodialyzer, cleaned, and transferred back into your body.
These sessions last about three to four hours, and they’re done in hospitals or independent dialysis centers three to four times a week. Patients remain stagnant while the process goes on, and the treatment takes up a solid chunk of your week every week.
In addition to the immobility, a problem with hemodialysis is the mortality rate associated with the treatment. A 2013 study that analyzed the effects of hemodialysis on patients with end-stage renal disease (ESRD)—the final stage of kidney failure, which we’ll discuss in moments—found that nearly 20 percent of those in the study died within two years while on hemodialysis. It’s also been found that only 35 percent of patients remain alive after five years after hemodialysis treatments.
This isn’t to say that hemodialysis doesn’t work, though. It’s an extremely effective treatment that helps patients prolong their lives and assists them while they wait on a kidney transplant—the only other effective treatment for kidney disease. Mortality rates have declined by nearly 30 percent since 1996, too, for both dialysis patients and transplant patients.
Various procedures doctors use to gain consistent access:
- Fistula: This is when a doctor joins an artery and a vein to make a large entryway for blood to leave and re-enter the body.
- Graft: When a fistula doesn’t work (if certain vessels are too far apart from one another), doctors may join arteries and veins in your body through the use of a plastic tube.
- Through the neck: For more immediate purposes, doctors may insert a catheter in a large vein in your neck to ensure they have a wide, free-flowing entryway for blood. This is usually temporary, though, until doctors can figure out where they will conduct future dialysis sessions.
Peritoneal Dialysis
In the peritoneal dialysis treatment process, patients take a much more inclusive role in the treatment and do much of the work on their own whether they are at work or home.
Within this treatment style, there are two different options patients can choose from:one with a machine in the presence of their own home; or one that is attached to your body that allows you to continue on with your day while the dialysis is occurring.
Continuous Ambulatory Peritoneal Dialysis (CAPD)
This treatment is done almost completely on your own. It’s called Continuous Ambulatory Peritoneal Dialysis because the treatment is made to be done while you can still walk around and work, thus the “continuous ambulatory” part of the name.
The process for CAPD starts with surgery, but it ends with the patient doing the rest of the work without having to visit a hospital or dialysis center. A surgeon will place a connection for a catheter in your abdomen area around your belly button, then every day, multiple times a day, you will manually hook up a cleansing fluid to the catheter and let the fluid do the cleansing work.
The bag of cleansing fluid should be placed above shoulder level whether you’re sitting down or standing up and walking around. The fluid then drains into your body and discharges the waste back into the bag. The bag of waste is then thrown away. The National Kidney Foundation says that this process should be done three to five times a day, depending on how much you weigh and the amount of function left in your kidneys, and each cleanse (formally called an “exchange”) takes about 30 to 40 minutes.
Automated Peritoneal Dialysis (APD)
This form of dialysis is similar to CAPD in that it can be done on your own time, but automated peritoneal dialysis is done with the help of a machine that is usually placed in your home.
The APD process begins the same as CAPD: a catheter is inserted in your abdomen near the belly button via surgery so you can connect the machine on your own. With APD, however, you must remain in the same spot for the entire process, like you would if you were participating in hemodialysis. Positive aspects of this treatment are:
- You can do this on your own time after work and on the weekends.
- You don’t need to wait in line at a dialysis center or hospital for an appointment.
- It can be done while sleeping so you don’t have to lose precious hours of the day.
- You don’t have to manually change out the bag after each exchange—just when you wake up and before you start the process again later in the night.
When Do I Need Dialysis?
Dialysis is necessary once 85 to 90 percent of your kidney’s functions are no longer working, thus you need dialysis to get most or all of the work done for them. However, you may not notice any symptoms of your kidneys working improperly until the the disease has nearly advanced to the final stage—kidney failure.
Dialysis is necessary once 85 to 90 % of your kidney’s functions are no longer working.
Kidney disease is the ninth leading killer in the United States, according to the American Kidney Fund, so it’s important to stay on top of your kidney health. This requires visits to the doctor and taking immediate concern if you notice any of the aforementioned symptoms of kidney disease.
How Does Dialysis Affect My Life?
Needing dialysis is a life-changing turn, but that does not mean you cannot still live a normal lifestyle. Because of the length of dialysis sessions (12 to 16 hours a week), it’s almost like having a part-time job, only you have to pay money at the end of every shift. But the whole point of dialysis is to get you feeling better, have your kidneys working properly, and rid yourself of the inhibiting health effects of kidney failure.
Dialysis treatment centers are available all around the United States, so outside of cutting into vacation time, you can still travel all around the country, whether it’s for leisure or work. Outside of times you need treatment, your life shouldn’t be inhibited once the treatment is done. Dialysis is meant to normalize electrolyte and waste levels in your blood, so once the filtered blood is in your system again, any health problems should subside until you near your next treatment.
Between dialysis sessions, you may be suggested to alter your diet to help keep blood sugar levels and blood pressure levels low. These dietary suggestions can include:
- Drinking Less Alcohol
- Eating More Vegetables and Fruits
- Smoking Less
- Eating Unhealthy Foods Less Often, Including Fast Food and Foods High in Sugar
- Regulating Mineral Intake, Like With Sodium, Potassium, and Phosphorus
The National Kidney Foundation notes that, while you may be able to return to work after dialysis treatments, you may want to avoid doing too much physical labor like heavy lifting. If you are in a field that requires it, you may want to look for a new line of work.
How To Pay for Dialysis
Dialysis is an expensive treatment, but luckily a lot of the treatment is covered by Medicare and insurance.
According to the Medicare website, they government covers a wide range of costs related to dialysis, including:
- Inpatient Dialysis Treatment (hemodialysis at a Medicare-approved hospital)
- Outpatient Dialysis Treatment (hemodialysis at an independent treatment center)
- Training for Self-Dialysis (CAPD and APD)
- Dialysis Equipment if You’re Treating Yourself at Home
The National Kidney Foundation says that Medicare covers about 80 percent of the overall cost of dialysis, while private insurance and individual payments cover the rest.
Some things not included in Medicare coverage are:
- Aides to help administer dialysis at your home
- Lost pay from having to take off work to have dialysis treatments
- An independent location to stay during dialysis treatment

